Physio Science: Insertional Achilles Tendinopathy
Insertional Achilles tendinopathy, retrocalcaneal bursitis, and Haglund’s disease are often discussed together as they are intimately related in pathogenesis and clinical presentation.
The Achilles tendon insertion, the fibrocartilaginous walls of the retrocalcaneal bursa that extend into the tendon, and adjacent cartilage-covered calcaneum form an ‘enthesis organ’. The key concept is that, at this site, the tendon, the bursa, and the bone are so intimately related that a prominence of the calcaneum greatly predisposes to mechanical irritation of the bursa and the tendon just proximal to the insertion, through both compression and tensile loads. Also, the mechanical load on this area is greater with dorsiflexion when the calcaneus impinges on the bursa and tendon. These mechanical loads lead to change in the nature of those tissues, consistent with the biological process of mechanotransduction (e.g. proprioception).
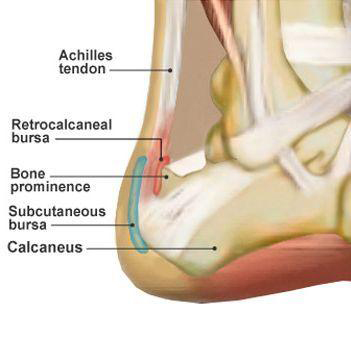
Haglund’s Deformity
Haglund-type calcaneus is a descriptive label for prominence of the posterolateral calcaneum. Haglund’s disease is a label for the clinical syndrome of a prominent, painful lateral portion of the tendon/bursa/calcaneus interface. Thus, an asymptomatic patient may be found to have a Haglund-type calcaneus on radiographs.
Common Causes
Haglund’s deformity can occur when there is frequent pressure on the backs of your heels. It may be caused by wearing shoes that are too tight or stiff in the heel. Since it often develops in women who wear pump-style high heels, Haglund’s deformity is sometimes referred to as “pump bump.”
You may also be more at risk for getting Haglund’s deformity if you have high foot arch, have a tight Achilles tendon, or tend to walk on the outside of your heel.
Treatment
This is a challenging condition to treat. Treatment must consider the enthesis organ as a unit. Isolated treatment of a bursitis is generally unsuccessful.
The treatment usually focuses on relieving pain and taking pressure off of your heel bone. Nonsurgical options include:
- Wearing open-back shoes
- Taking non-steroidal anti-inflammatory drugs (NSAIDs), such as Ibuprofen
- Icing the bump for 3 x 15 minutes per day to reduce swelling
- Specific loading exercises
- Getting a soft tissue massage to release calf trigger points
- Orthoses prescription, specifically those with high arches
- Wearing heel raises to reduce compressive loads, reducing dorsiflexion
- Wearing heel pads to reduce pressure from your shoes
- Getting ultrasound treatment
- Extracorporeal shockwave therapy (ESWT)
- Wearing an immobilizing boot or cast during periods of severe pain.
Surgery can also be used to treat Haglund’s deformity if less invasive methods don’t work. During surgery, your doctor will remove the excess bone from your heel. The bone may also be smoothed and filed down.
This reduces the pressure on the bursa and soft tissue. You may be given a general anesthesia that will put you to sleep during the surgery. This is usually done if your Achilles tendon is damaged and your doctor needs to fix it.
After surgery, it will take up to eight weeks for your wound to completely heal, although rehabilitation can take 3-12 months. Your doctor will likely give you a boot or cast to protect your foot. You may also need to use crutches for a few days.
The cut will have to remain bandaged for at least seven days. Within two weeks, your stitches will be removed. Your doctor may want to get an X-ray of your foot on follow-up visits to ensure that it’s healing properly.
Prevention
You can lower your risk of developing Haglund’s deformity by taking care of your feet. Try to:
- Avoid shoes with tight, stiff heels, especially for long periods of time
- Avoid running on hard surfaces or uphill
- Wear open-back shoes
- Wear fitted, padded socks with non-slip soles
- Wear prescribed orthoses
- Perform stretching exercises to prevent tightening of the Achilles tendon.
To book an appointment with one of our therapist please visit our online book service here.
For more information about our clinics you can visit our clinic page here.